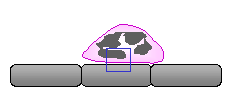
Firm Adhesion
 It
is thought that most if not all leukocytes adhere only after having rolled.
Several studies suggest that direct adhesion (from the free-flowing leukocyte
pool) is extremely rare. E-selectin participates
in the conversion of rolling to firm adhesion. E-selectin deficient mice
have a reduced number of firmly adherent leukocytes in response to local
chemoattractant (Ley
et al., 1998) or cytokine stimulation (Milstone
et al., 1998). This defect may be related to the more rapid rolling
velocities in the absence of E-selectin (Kunkel
and Ley, 1996).
It
is thought that most if not all leukocytes adhere only after having rolled.
Several studies suggest that direct adhesion (from the free-flowing leukocyte
pool) is extremely rare. E-selectin participates
in the conversion of rolling to firm adhesion. E-selectin deficient mice
have a reduced number of firmly adherent leukocytes in response to local
chemoattractant (Ley
et al., 1998) or cytokine stimulation (Milstone
et al., 1998). This defect may be related to the more rapid rolling
velocities in the absence of E-selectin (Kunkel
and Ley, 1996).
Interfering with CD18 integrin function is
one of the most efficient ways to curb leukocyte recruitment in many forms
of experimental inflammation. Although the response to exogenous chemoattractant
is drastically reduced when CD18 is absent or not functional (
Scharffetter-Kochanek et al., 1998; Arfors
et al., 1987), cytokine treatment still yields a robust inflammatory
response in gene-targeted mice lacking CD18 (Jung
et al., 1998). This suggests that CD18 integrins participate in leukocyte
arrest, but are not always required. Neutrophils express small amounts
of other integrins, including VLA-4
( 41 integrin) (Kubes
et al., 1995), which may be important in these alternative pathways.
However, CD18 deficient mice have severe inflammatory defects including
skin ulcerations, elevated neutrophil counts and immunoglobulin levels,
increased susceptibility to streptococcus pneumoniae, and a severe
defect in leukocyte adhesion and T-cell activation (Scharffetter-Kochanek
et al., 1998), a defect in leukocyte recruitment to peritonitis (Walzog
et al., 1999) and a lack of neutrophil recruitment to the skin (Mizgerd
et al., 1997). Patients lacking CD18 expression suffer from leukocyte
adhesion deficiency type 1 (LAD-1). When CD18 is totally absent, LAD-1
is a very severe disease, which can lead to early lethality (Anderson
and Springer, 1987).
41 integrin) (Kubes
et al., 1995), which may be important in these alternative pathways.
However, CD18 deficient mice have severe inflammatory defects including
skin ulcerations, elevated neutrophil counts and immunoglobulin levels,
increased susceptibility to streptococcus pneumoniae, and a severe
defect in leukocyte adhesion and T-cell activation (Scharffetter-Kochanek
et al., 1998), a defect in leukocyte recruitment to peritonitis (Walzog
et al., 1999) and a lack of neutrophil recruitment to the skin (Mizgerd
et al., 1997). Patients lacking CD18 expression suffer from leukocyte
adhesion deficiency type 1 (LAD-1). When CD18 is totally absent, LAD-1
is a very severe disease, which can lead to early lethality (Anderson
and Springer, 1987).
Among the 2 integrins, only LFA-1 and Mac-1
have been investigated in vivo. Intravital microscopic studies suggest
that LFA-1 is the most important 2 integrin in firm leukocyte adhesion
(Schmits
et al., 1996), while Mac-1 has no apparent role in adhesion, but seems
to be important in neutrophil activation and phagocytosis (Lu
et al., 1997). Nothing is known about the role of the  x
(p150,95) and
x
(p150,95) and  d chains
(CD11c and CD11d) in leukocyte adhesion or recruitment in vivo.
d chains
(CD11c and CD11d) in leukocyte adhesion or recruitment in vivo.
In cytokine-induced inflammation, slow-rolling
leukocytes do not stop abruptly, but show a gradual decrease of their
rolling velocity before becoming adherent (Kunkel et al., 2000). This
deceleration is strictly dependent on CD18 integrins
(Kunkel et al., 2000). Since rolling leukocytes show a graded elevation
of intracellular free calcium while rolling more and more slowly, it appears
that rolling leukocytes are partially activated before arrest. This process
appears to take about one minute or more. Although IL-8 receptor is known
to be involved, signaling through adhesion receptors, for example L-selectin (Steeber
et al., 1997), may also contribute to this process of physiological
leukocyte recruitment.
LFA-1 and Mac-1 both
can bind to ICAM-1 and ICAM-2 (Xie
et al., 1995; Diamond
et al., 1990; Staunton
et al., 1989; Dustin
and Springer, 1988). A role for ICAM-2 in leukocyte recruitment has
not been demonstrated so far. ICAM-2 deficient mice show a prolonged eosinophilic
infiltrate in a model of allergic lung inflammation, but have no inflammatory
defect (Gerwin
et al., 1999). ICAM-1 have a mild inflammatory defect (Sligh,
Jr. et al., 1993), not comparable with that seen in CD18 deficient
mice. Although it has been argued that alternatively spliced forms of
ICAM-1 found in these mice (King
et al., 1995) may allow for residual leukocyte binding, these isoforms
are only found in thymus and spleen and not in inflamed organs. Recently,
an ICAM-1 null mouse has been produced (R.G. Collins and A.L. Beaudet,
unpublished information) that should bring definitive answers with respect
to the role of ICAM-1 in inflammation. Leukocytes rolling in resting inflamed
venules require ICAM-1 to stop in response to a chemoattractant
(Argenbright
et al., 1991). However, ICAM-1 is no longer required after activation
with inflammatory cytokines (Foy and Ley, 1999; Ley
et al., 1998), suggesting that other, unknown endothelial ligands
for 2 integrins must exist.
Monocytes, eosinophils, and many lymphocytes express  41
integrin (VLA-4) (Hynes,
1992), and mouse and rat neutrophils also express small amounts (Kubes
et al., 1995). When other adhesion molecules are unavailable,
41
integrin (VLA-4) (Hynes,
1992), and mouse and rat neutrophils also express small amounts (Kubes
et al., 1995). When other adhesion molecules are unavailable,  41
integrin can mediate both leukocyte rolling
(Berlin
et al., 1995; Sriramarao
et al., 1994; Alon
et al., 1995) and firm adhesion.
41
integrin can mediate both leukocyte rolling
(Berlin
et al., 1995; Sriramarao
et al., 1994; Alon
et al., 1995) and firm adhesion.  41 integrin
binds to endothelial VCAM-1 (Luscinskas
et al., 1995) and alternatively spliced fibronectin (Guan
and Hynes, 1990). Intravital microscopic evidence available to-date
suggests that most
41 integrin
binds to endothelial VCAM-1 (Luscinskas
et al., 1995) and alternatively spliced fibronectin (Guan
and Hynes, 1990). Intravital microscopic evidence available to-date
suggests that most  4-dependent binding is
through VCAM-1, because antibodies to VCAM-1 applied in the microcirculation
(U. Jung and K. Ley, unpublished observations) and in atherosclerotic
arteries (Ramos
et al., 1999) block leukocyte rolling and adhesion to a similar extent
as
4-dependent binding is
through VCAM-1, because antibodies to VCAM-1 applied in the microcirculation
(U. Jung and K. Ley, unpublished observations) and in atherosclerotic
arteries (Ramos
et al., 1999) block leukocyte rolling and adhesion to a similar extent
as  4 antibodies. Since homozygous α4
(Yang
et al., 1995) or VCAM-1 (Gurtner
et al., 1995) deficient mice die before birth due to morphogenetic
failure unrelated to the inflammatory function of these molecules, definitive
answers for the roles of these two adhesion molecules await the generation
of tissue-specific and/or inducible null mutants.
4 antibodies. Since homozygous α4
(Yang
et al., 1995) or VCAM-1 (Gurtner
et al., 1995) deficient mice die before birth due to morphogenetic
failure unrelated to the inflammatory function of these molecules, definitive
answers for the roles of these two adhesion molecules await the generation
of tissue-specific and/or inducible null mutants.
Comment on this page's content or view comments made by others!